Federal Safety Net Drug Pricing Program Leaves Rural Patients and Seniors Behind
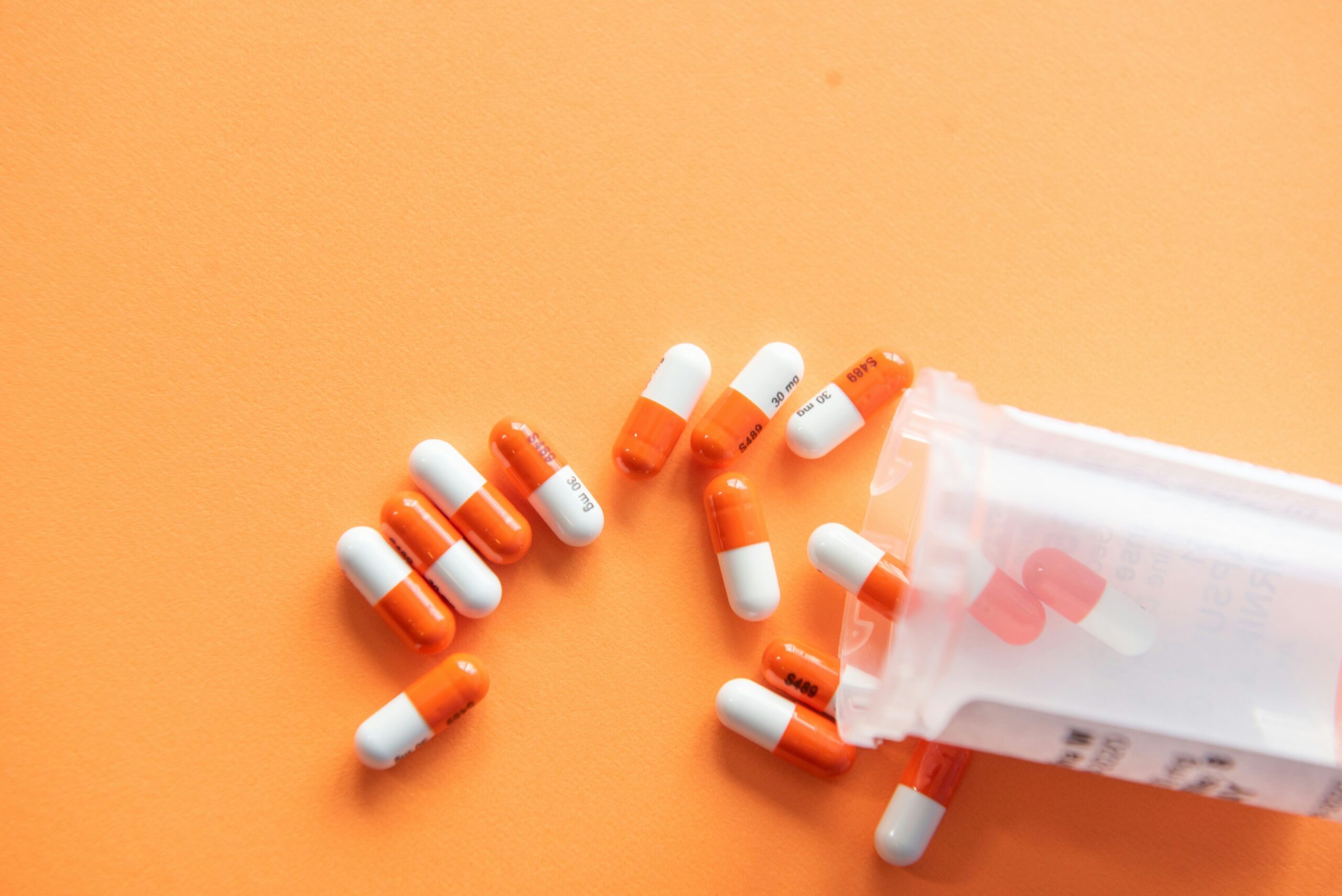
Featured Photo Credit: Unsplash/Christina Victoria Craft
Click here to read this Op-Ed on realclearhealth.com
Despite improvements in the quality and delivery of health care in America, rural Americans still face daunting barriers to accessible treatment. Across the board, rural Americans suffer from unique health challenges compared to those living in urban areas, often spending more on health care while also having less access to doctors and hospitals. The health access challenges are only growing as the rates of older Americans living in rural areas rapidly increases. There are federal programs in place that are intended to provide support to rural and senior communities, but recent data are highlighting how hospitals are using the program to boost profits instead of transferring the benefits to rural patients.
The 340B Drug Pricing Program was created by Congress 30 years ago—it enables nonprofit healthcare entities to buy prescription drugs at discounted prices with the intention of transferring that savings on to patients through discounted medications or providing care at low or no cost. The 340B program has grown substantially over the years, but most patients aren’t seeing the benefits. Instead, there is evidence that hospitals and contract pharmacies are exploiting the program through dwindling charity care rates and a rural designation loophole to reap profits from affluent communities while leaving rural Americans and seniors behind.
One way that Congress envisioned profits from the 340B program to be used is through increased levels of charity care to serve low-income and uninsured communities. However, evidence has shown that 340B hospital profits are on the rise, but charity care levels have been declining in recent years. A recent study found that an estimated 85% of disproportional share hospitals (DSHs), a type of hospital that commonly gets these drug discounts, earned more in 340B profit than they spent on charity care costs.
Another way for hospitals to qualify for 340B discounts besides a DSH qualification is to be designated as a “Rural Referral Center,” or RRC. It was designed to help nonprofit hospitals serving low-income populations reinvest the savings into the health and wellbeing of rural communities. Notably, the threshold of low-income patients is much more lenient in the RRC designation as opposed to more traditional pathways to the 340B program. However, the law doesn’t require that RRC designated hospitals be in rural areas or treat rural patients. In fact, 82% of currently enrolled RRCs are in urban areas, and less than a quarter of patients treated live in rural areas.
RRCs have also grown substantially in recent years—according to a recent study by the Berkeley Research Group, RRCs have grown more than twice the rate of the overall 340B program with a 405% increase since 2017, and these hospitals are also ramping up 340B discounted drug purchases faster than any other type of 340B hospital. Additionally, RRCs are one of the many 340B covered entities that contract with pharmacies that, on average, are located in much wealthier zip codes than the 340B hospital. Some of the largest hospitals in the largest urban areas of our country are abusing the 340B program by calling themselves “rural” to avoid the more stringent requirements of urban hospitals to serve a higher percentage of low-income patients.
Rural communities often are home to a much higher percentage of senior Americans and Medicare beneficiaries. A recent analysis from an independent, non-partisan commission of experts focused on the Medicare program found that both Medicare and its beneficiaries overpaid by nearly $4 billion for medications subject to the 340B Program by exceeding 340B ceiling prices – to put it simply, 340B hospitals receive billions in profit while Medicare patients foot the bill.
Reaping the benefits of the 340B program without helping rural patients in need is reprehensible, especially considering the health access barriers rural Americans face every day. Rural areas are home to more low-income and uninsured patients, creating financial strain on those seeking treatment. Shortages of healthcare workers in rural communities also contributes to worsened health outcomes—data show that less than 8% of physicians choose to practice in rural settings, and this shortage of workers is only likely to worsen in the next decade. The health providers in these rural areas are often difficult to access, as reliable transportation can also be a barrier for rural residents due to long distances, poor road conditions, and the limited availability of public transportation.
The intentions of the 340B program are honorable, but the program has clearly veered far off course. The 340B program’s lax rules incentivize urban hospitals to attain RRC designations to profit from drug discounts without fulfilling their obligation to support rural Americans. Congress has a responsibility to increase accountability within the safety net program so that rural patients are not left behind.
Sincerely,